From Basics to Benefits: A Clear-Cut Guide to FHIR VS. HL7

In the past two decades, healthcare has witnessed cardinal changes, moving from traditional paper documentation to advanced healthcare software solutions. The once-restricted access to medical information has been improved due to this digitalization. Yet, the real leap in the health data exchange field made HL7 and FHIR standards. FHIR, while part of HL7, differs from it substantially. That’s why comparing FHIR vs. HL7 is quite important for healthcare organizations looking to improve data-sharing capabilities within their IT systems.
Leveraging Relevant Software’s decade of industry experience, we have created a detailed comparison of HL7 vs. FHIR, highlighting their key differences, benefits, and features to help you choose the most suitable option for your organization.
Importance of Healthcare Interoperability
Healthcare organizations have long recognized the crucial need for data interoperability to ensure consistency, clarity, and enhanced understanding across medical records. The need for it was also emphasized by the negative experiences 32% of patients had due to the absence of medical data interoperability. However, achieving this has been a challenge due to a lack of means, strategies, and commitment.
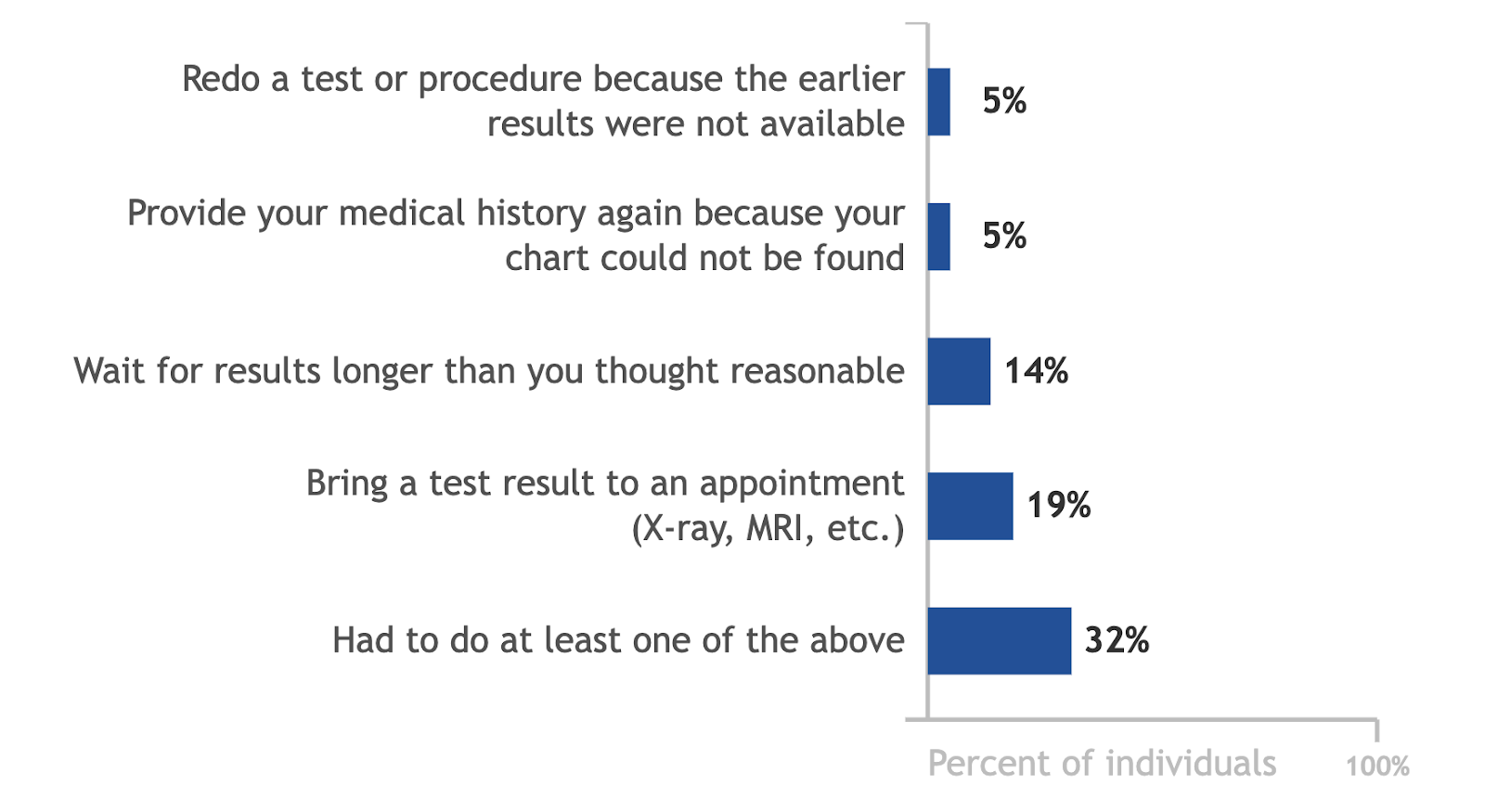
Image credit: Healthit
However, the shift has gained momentum with the enforcement of the Cures Act Final Rule, and many organizations are now ready to embrace data interoperability. Specifically, over half of health system CIOs plan to allocate an additional 5-20% of their budgets to interoperability initiatives in 2023. The increased investments, in turn, drive the growth of the market for healthcare interoperability solutions, which is expected to jump from $3.4 billion in 2022 to $6.2 billion by 2027.
In practical terms, interoperability is the glue that connects health records and translates them into a consistent format to make them more accessible and transferable across different healthcare systems. The FHIR standard, along with HL7, plays one of the major roles in this.
HL7 – Health Level Seven International: Overview
Health Level Seven International, commonly known as HL7, can be referred to as either a healthcare-related organization that develops international standards for exchanging, sharing, and retrieving electronic health information or HL7 standards themselves. And further in the article, we’ll talk specifically about those standards. So, here’s a short overview of HL7 – the first framework for data exchange that appeared in the healthcare industry.
History and Evolution of HL7
Founded in 1987, HL7 aimed to set global standards for healthcare data exchange. The initial HL7 V2, introduced in 1989, marked significant progress in driving enterprise-level interoperability and was widely adopted by many healthcare companies. But, as the influence of data on streamlining clinical workflows grew in the early 2000s, HL7 V2 could not cope with it, and the world saw the emergence of the more advanced, XML-based HL7 V3. This, however, due to the lack of backward compatibility and complex implementation, didn’t find widespread adoption. Then came CDA and, later on in 2014, the FHIR standard protocol, which we’re discussing in this article.
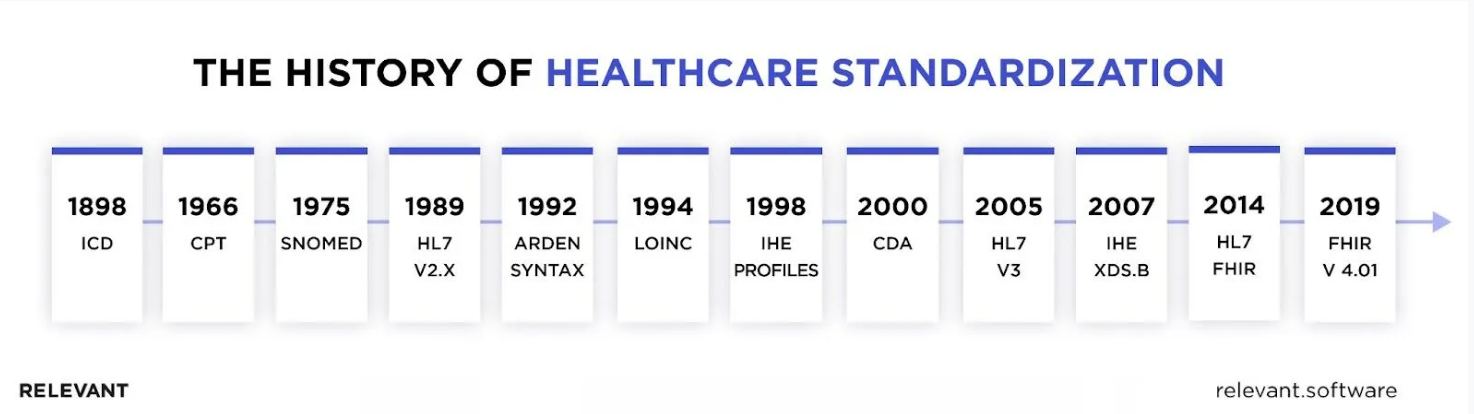
The evolution of HL7, from its initial stages to the development of FHIR, illustrates a continuous commitment to meet the growing demands of the healthcare sector. Each version developed by HL7 was meant to simplify communication between health applications, reduce administrative complexities, and improve healthcare delivery quality.
HL7 Standards
As we now know, there were a few versions of HL7 standards. But when someone mentions HL7, they often mean V2, as this version has gained the widest adoption – 95% of US medical organizations use it! That’s why we’ll review and compare this version and refer to V2 when talking about HL7 standards to avoid confusion.
So, introduced in 1989, the HL7 V2 messaging standard has been a cornerstone in establishing healthcare interoperability and laid the groundwork for modern communication between systems within hospitals. It addresses both structural and semantic requirements of IT healthcare systems, containing specifications essential for clinical, administrative, financial, and logistical processes. Designed to support centralized patient care infrastructure, it places less emphasis on data exchange, a contrast evident when comparing HL7 V2 vs. FHIR.
Use Cases in Healthcare
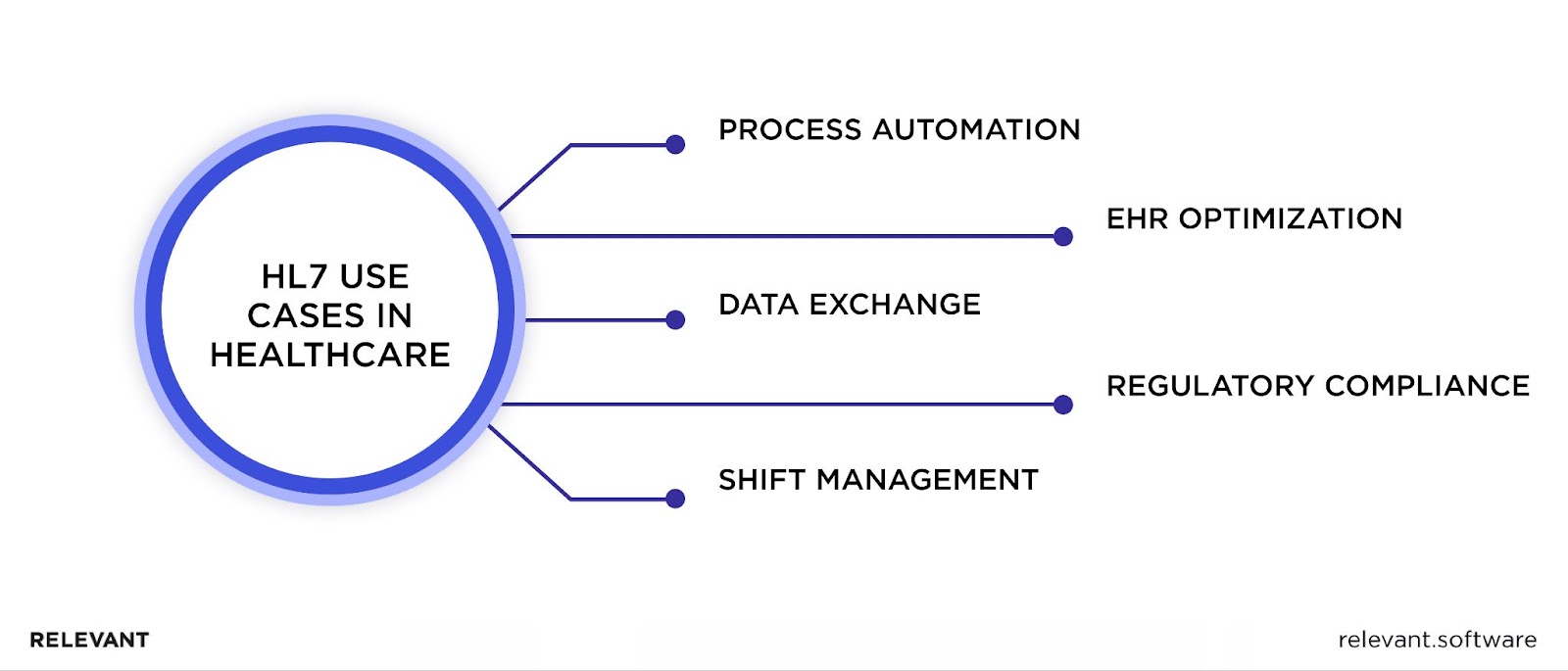
HL7 sounds like a promising solution in theory, but let’s see the real applications of it. Considering its large user base, there are enough use cases.
- Automating processes. HL7 integration helps medical institutions save big on administrative costs by minimizing manual labor, automating repeated tasks, and mitigating errors in procedures such as data entry and lab testing.
- Optimizing Electronic Health Records (EHR). HL7-compliant EHRs improve patient data access and management, providing healthcare professionals with accurate and current information for comprehensive treatment. This is particularly beneficial for incoming patients, as the ability to integrate HL7 data from EHR systems from different medical facilities saves time and enhances patient care.
- Exchange of information between healthcare organizations. Facilitating a continuous flow of electronic health data between medical facilities, HL7 allows hospitals to exchange medical information during patient transfers easily.
- Regulatory compliance. HL7 simplifies information sharing with regulatory bodies to meet public health reporting standards. For example, biopharmaceutical companies and manufacturers of medical devices can easily share specifications with regulators.
- Healthcare workers’ shift management. Having real-time data on staff workload provided by HL7, healthcare organizations can fairly and efficiently distribute shifts based on caregivers’ qualifications and patient load.
Advantages and Challenges of HL7
Facilitating communication between different systems, HL7 has helped medical facilities overcome some of the complex and costly software development that was necessary to create interfaces for systems interaction in the past. Plus, healthcare organizations saw the true value in V2 flexibility, as it allows systems to support messages selectively, decide which segments to use, and even introduce custom segments. Despite being the most widely implemented healthcare standard, HL7 isn’t without drawbacks.
While HL7 V2 was designed with high flexibility and customization in mind, this characteristic also presents itself as a disadvantage. The standard’s ambiguity and excessive flexibility, along with its generic nature, do not allow for constraints for specific use cases, leading to inconsistencies, overlaps, and non-specific compliance in handling clinical data.
Also, HL7 is ill-equipped to support the latest tech solutions in healthcare. The absence of a clear message model, a semantic framework, and a standard method for extensions means that achieving interoperability requires organizations to depend significantly on custom coding, site-specific installation parameters, and interface engines, potentially leading to compatibility issues.
Your next read: HL7 certification
FHIR – Fast Healthcare Interoperability Resources: Overview
Fast Healthcare Interoperability Resources, better known as FHIR, is a newer, more flexible, and adaptable standard. It uses modern web technologies to allow the exchange of administrative and clinical data. FHIR was also designed to be easier to implement and maintain than HL7 while being compatible with most web-centric platforms. In part due to this, FHIR is capturing the attention of healthcare organizations. So, let’s take a closer look at it.

History and Development of FHIR
The development of FHIR began in 2012 under the HL7 umbrella, aiming to create a completely new way of patient data exchange in healthcare. By 2014, after multiple refinements, HL7 FHIR saw its draft for trial use, accessible to all. Over the next few years, FHIR’s development tackled the challenges of healthcare interoperability by allowing developers to design apps using modern web technologies like HTML, JSON, XML, and OAuth. Since FHIR found adoption across EHRs and the US government, tech giants such as Google, Apple, and Microsoft joined the movement as well. The community continues developing additional FHIR specifications, such as the authorization framework SMART on FHIR.
FHIR, an acronym that aptly sounds like “fire,” blends the strengths of HL7’s v2, v3, and CDA to introduce a newer and simpler model for electronic exchange. While it’s definitely the best HL7 solution, FHIR is still maturing. Healthcare organizations may face data integrity challenges, while the shift from older systems could be discouraging. However, with the right partners, HL7 FHIR implementation is much easier and trouble-free.
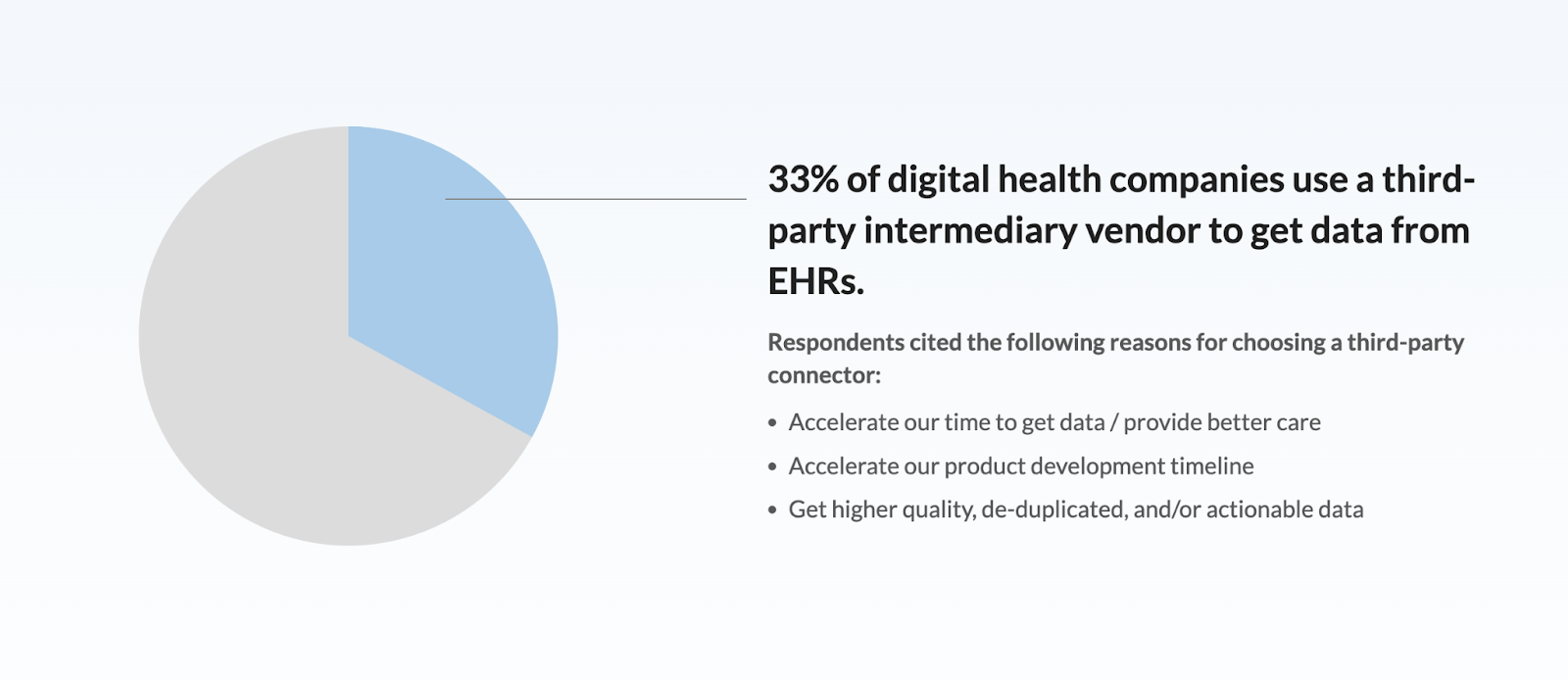
Image credit: Healthgorilla
FHIR Standards
The healthcare FHIR standard is capable of everything HL7 V2 is and even more. Designed to universalize electronic records and data formats while being easily implemented across mobile and web-based platforms, FHIR, in fact, makes adopting healthcare interoperability much simpler for medical institutions. Comparing FHIR vs HL7 V2, the first isn’t limited to a single encoding format. On top of that, FHIR provides better security features, faster implementation, and one-to-many data exchange options. For healthcare organizations, it means less time to integrate third-party applications and make them work seamlessly.
As for FHIR’s tech characteristics, it uses popular and widely applied technologies most developers know and work with. It employs a client-server model for data exchange, enriched by REST architecture, and communicates using common data formats like XML, JSON, and RDF through HTTP APIs. It minimizes the inconsistencies often seen in HL7 V2 implementations by clearly defining the standard protocol and maintaining healthcare terminologies. Furthermore, FHIR champions reusability, allowing data objects to be adjusted independently.
Use Cases in Healthcare
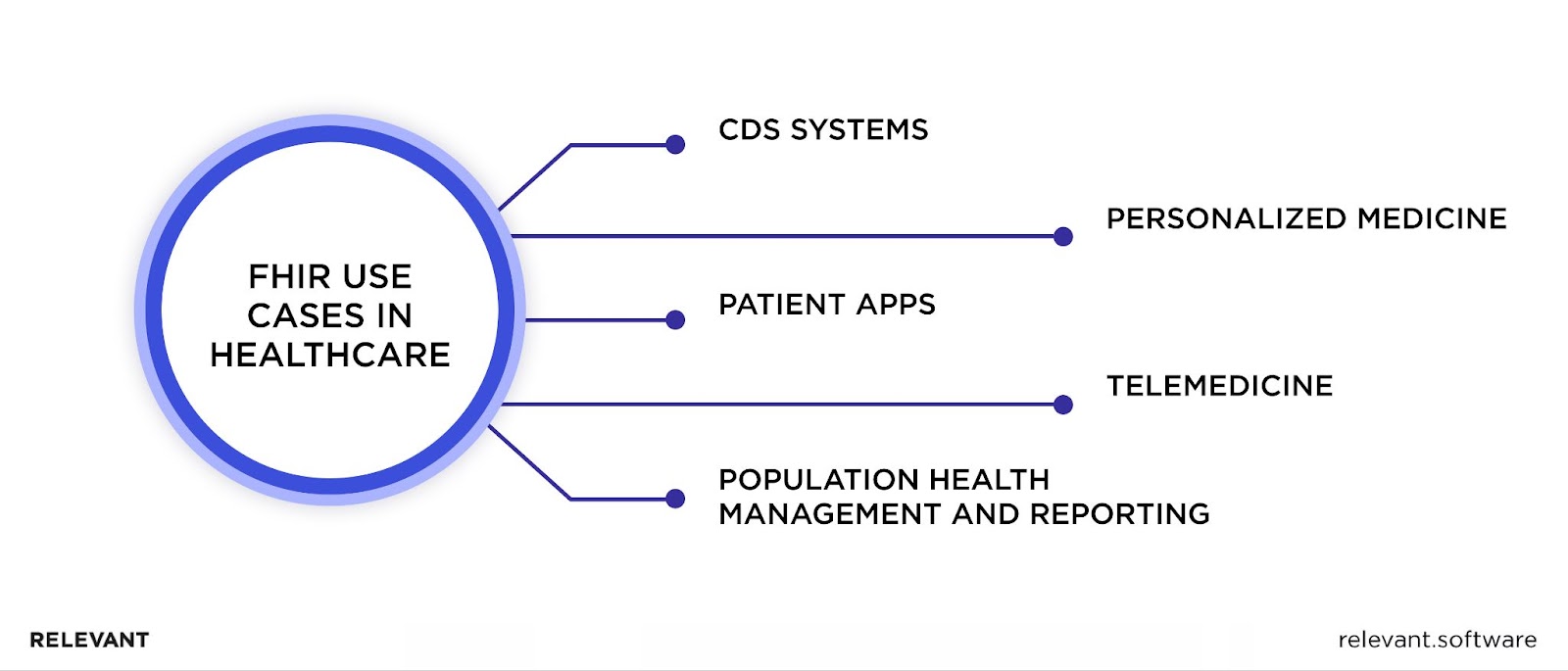
No doubt, FHIR, with its advanced capabilities, has pushed the boundaries of health IT and found new applications in healthcare that advance processes through seamless data interchange. So, here are its diverse use cases:
- Clinical Decision Support (CDS) Systems. FHIR integrates with CDS tools to provide clinicians with real-time patient data from EHR systems and drive evidence-based treatment decisions.
- Personalized medicine. By accessing comprehensive patient histories via FHIR, doctors can tailor therapeutic interventions to individual needs.
- Patient applications. This framework supports interactive apps, allowing patients to access information from healthcare providers’ EHRs, monitor metrics, and engage with doctors.
- Population health management and research. Since FHIR facilitates health data exchange, it helps researchers identify health trends and disparities across populations.
- Telemedicine. Better remote care is possible due to smoother patient data transmission to telemedicine platforms enabled by FHIR, which drives informed decisions during virtual consultations.
Advantages and Challenges of FHIR
By streamlining the healthcare data exchange, FHIR makes it simpler for doctors and administrators to share patient information, even when using disparate software systems. At the core of the FHIR standard is the concept of unique identifiers for every resource. Much like how URLs direct users to specific web pages across different browsers or devices, FHIR ensures easy access to the correct data from any application or device.
By establishing standard URLs for distinct data packets, FHIR eliminates the need for continuous back-and-forth document exchanges between systems, ensuring that apps reference the same information simultaneously. This adaptability, combined with its integration with web services, allows developers to create intuitive applications that provide fast and dependable access to relevant data, regardless of the EHRs or applications in play. Moreover, its ability to support numerous data formats broadens its applicability across different tech environments.

Yet, FHIR isn’t without challenges. Its flexibility, while beneficial, can sometimes lead to inconsistencies in implementation, potentially causing data discrepancies. These challenges are further compounded when different healthcare systems use different versions. Moreover, when EHR vendors either partially implement or don’t fully integrate the available FHIR APIs, it creates discrepancies that hinder the ultimate goal of achieving seamless interoperability across platforms.
FHIR vs. HL7 – A Comprehensive Comparison
Both aim to standardize the way patient information is shared, yet due to the different underlying technologies, they approach this goal distinctly. So, we analyzed the tech details of each framework to provide side-by-side HL7 standards vs. FHIR comparison and help you decide which might best serve your specific healthcare needs.
Architecture and Design
FHIR adopts a RESTful architecture, which facilitates data transmission over HTTP using standard CRUD operations and allows handling large data volumes from various interfaces. Coupled with modern web services, FHIR helps different healthcare platforms and technologies interact seamlessly and share data in real-time effortlessly. Moreover, FHIR’s granular data elements, known as “resources,” store clinical data in a structured format, making it easily accessible and manageable.
Conversely, traditional HL7 operates on a segment-based structure, where data is exchanged in a predefined format, ensuring that each piece of information resides in a specific, pre-allocated segment. HL7’s design, while robust and widely used, can sometimes introduce complexity due to its rigid structure and the necessity for precise parsing and interpretation. This stark contrast in design philosophy between FHIR vs. HL7 message types shows the evolution, moving from a stringent, message-based model to a more flexible, web-based approach.
Interoperability Comparison
HL7 V2 vs. FHIR in terms of interoperability notably contrasting. HL7 V2 was a significant stride in its time that allowed healthcare systems to communicate. However, the segment-based structure of HL7 and its flexibility often led to varied custom implementations, sometimes creating challenges in achieving seamless data exchange.
On the other hand, FHIR, with its modular design, web-based, and open standards, offers a simpler way to reach healthcare interoperability. By defining distinct “resources” for different data elements and using easily integrated web technologies, FHIR ensures that data can be accessed, handled, and shared across diverse systems with relative ease.
Efficiency and Performance Analysis
Since HL7 employs a segment-based message structure, which, while effective for many legacy systems, it can lead to extended messages and slower data transmission in high-transaction settings. In contrast, FHIR’s resource-based approach optimizes data exchanges by supporting XML and JSON. FHIR minimizes data redundancy and speeds up data retrieval and transfer thanks to its design.
Security and Compliance
While HL7 employs transport layer security for data protection, FHIR extends its security measures by incorporating both transport layer security and SSL. And it also uses a specific authorization protocol for more secure information exchange between doctors and patients.
In terms of compliance, FHIR’s robust security features align well with newer strict regulatory demands, guaranteeing that patient information remains confidential and is only accessed by authorized individuals. HL7 has been a trusted standard for years, but the constantly changing regulations require continuous updates and adaptations.
Adoption and Community Support
Having been around for decades, HL7 has gained a large user base, with many healthcare systems and institutions relying on its protocols for data exchange needs. The extensive use of HL7 has led to a large community of developers, users, and supporters who create and share resources and expertise to troubleshoot arising issues and keep the standard relevant.
Although FHIR is a newer framework, it’s rapidly gaining traction. Its modern design, which uses popular web technologies, attracts many developers and lowers the barrier to entry. As a result, the FHIR community is rapidly growing and contributes to spreading the framework adoption. More institutions are considering shifting from traditional HL7 standard protocol to embrace FHIR’s capabilities.
FHIR vs. HL7: The Comparison Table
To summarize all the characteristics and differences of the FHIR VS. HL7 format discussed above, we’ve prepared a comparison table highlighting the essential aspects.
| HL7 | FHIR | |
| Structure | Based on messages built with pipes, text, and hats | REST APIs access |
| Flexibility | Flexible | More flexible |
| Extensibility | Non-extensible | Feature extensible resources |
| Security | Transport layer | Transport layer and SSL, authorization protocol |
| Platform support | EHR, HIS, EMR, LIMS | EHR, HIS, EMR, LIMS, telemedicine, mobile apps |
| Use cases | Management of medical records | Universal sharing of healthcare information across mobile health apps and IoMT devices |
| Interoperability type | Syntactic | Syntactic and semantic |
| Human readability | No support | Supports |
| Compatibility | Compatible with all HL7 V2 features | Not compatible with HL7 V2. Backward compatibility with HL7 CDA and V3 |
| Costs | Cheap | Cheap if it’s not a migration from HL7 older versions |
| Adoption | Very popular. 95% of US medical organizations use it | Still at an early stage but is set to take the lead |
| Learning | A big learning curve | Weeks to learn and adopt |
Deciding on the right standard for achieving interoperability will depend on your current resources and goals. If you seek adaptability and new advancements, FHIR is what you need. However, if you’re looking for tried-and-true solutions, other HL7 versions might align better with your needs. As a healthcare IT consulting company, we’d almost always advocate for FHIR. Read further why, in the HL7 V3 vs FHIR and HL7 CDA vs. FHIR battle, the latter often gets our nod.
FHIR VS. HL7: Why FHIR Is Better than HL7
Given that FHIR is the latest standard that incorporates critical improvements of HL7’s previous versions, it’s no surprise that numerous healthcare organizations find it beneficial. Here are the features and benefits that make FHIR stand out among its mature counterparts:
- Ease of Implementation. FHIR is designed with modern technologies in mind, making it more intuitive for developers. Its compatibility surpasses that of HL7 standards, and its primary aim is to simplify interoperability. FHIR is not just about exchanging data but ensuring it’s done seamlessly across different platforms.
- Versatility and cost-effectiveness:
- FHIR caters to a broad spectrum of scenarios. Its resources give developers the tools to tailor healthcare systems to specific administrative and clinical needs.
- The RESTful API support ensures FHIR’s adaptability with mobile applications, which is crucial for real-time data access and exchange.
- One of FHIR’s standout features is its free accessibility. All essential resources for its implementation are available at no cost, reducing the financial barriers to adoption.
- Its design promotes data governance, giving providers and patients greater control over data, enhancing security, and facilitating smoother information exchanges.
- Optimized for modern healthcare demands:
- Unlike HL7, where segments are rigid, FHIR allows for independent manipulation of referenced objects, adding depth to data referencing.
- The architecture of FHIR is streamlined, addressing the clutter often seen in HL7’s previous standards. By adhering to the 80-20 principle, it focuses on the most critical elements and covers a vast majority of healthcare needs. Yet, it remains flexible enough to accommodate specific requirements through controlled extensions.
- FHIR integrates profiles into the core methodology and tooling, which multiplies their effectiveness and utilization.
These advantages are rather convincing for opting for FHIR over alternative options. It helps healthcare organizations better adapt to rapid shifts in interoperability demands. Of course, FHIR isn’t without its flaws, but it’s currently the top choice for most healthcare software engineers.
FHIR VS. HL7: Bottom line
Selecting the right standard is crucial for efficient and high-quality healthcare delivery. The choice between FHIR vs. HL7 is challenging, and it’s a very important decision for healthcare institutions because the transition between these standards isn’t a simple task.
Yes, HL7 V2 remains the most popular and widespread framework in the healthcare sector. However, FHIR stands out due to its improved data exchange capabilities and mobile compatibility. Its forward-thinking design and integration with current web technologies offer a fresh perspective and open doors to endless opportunities.
Fortunately, it doesn’t have to be a solo decision. You may need a reliable healthcare software development partner like Relevant Software to help you pick the best option and develop a strategic approach to health record standardization. Contact us to get on the path to healthcare interoperability and reap the benefits of seamless data exchange.
Also, read more about nanobots in medicine.
